_Jonathan Purtle
Purtle is an assistant professor in the Department of Health Management and Policy in the School of Public Health.
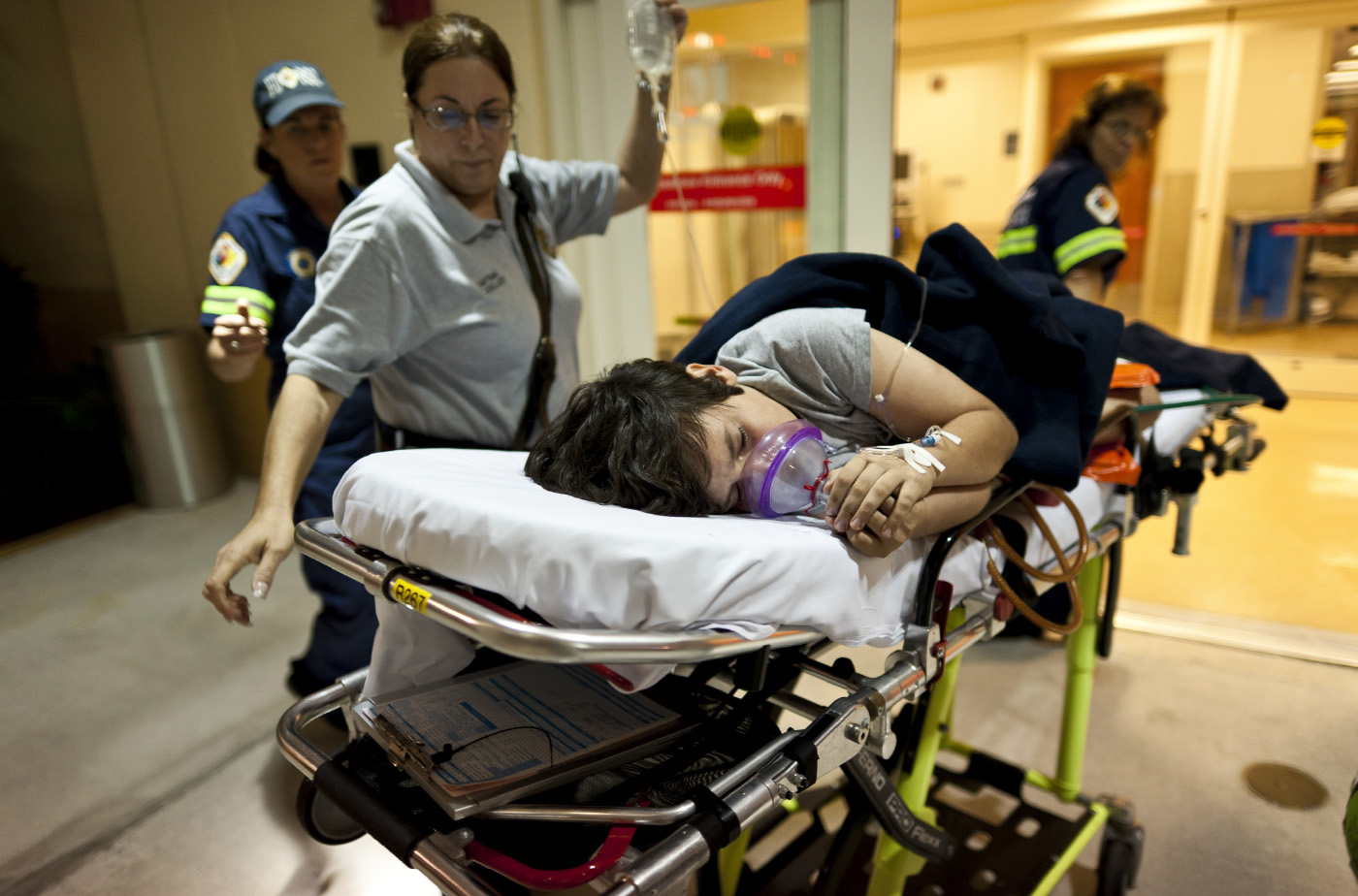
The best time to stop cycles of violence is at the moment of crisis, when tensions are highest. Usually, that means inside the emergency room. Nationwide, more than 25 hospitals have adopted intervention programs to prevent violent injuries before they happen.
Through hospital-based violence intervention programs (HVIPs), teams of medical professionals and social workers step in at a critical moment in a patient’s life — the period following a violent injury such as a gunshot or stab wound — with case management, counseling and other services to help them escape the cycle of violence.
Emergency_Action
Attaching dollars and cents to hospital-based violence intervention programs is important because many lack sustainable funding sources.
As these programs have grown, so too have reports of their success. There is evidence that HVIPs prevent violent reinjury and perpetration, reduce aggressive behaviors and improve employment, education and health-care utilization among program participants.
And, according to a Drexel research team, not only do these programs transform lives, there can be significant cost savings in various sectors including health care and criminal justice.
The team reports in the February issue of the American Journal of Preventive Medicine that an HVIP serving 90 clients could result in cost savings from tens of thousands of dollars and up to about $4 million in a five-year period.
“This is the first systematic economic evaluation of a hospital-based violence intervention program, and it’s done in a way that can be replicated as new evidence emerges about the programs’ impacts across different sectors,” says Jonathan Purtle, who was lead author of the simulation study.
Attaching dollars and cents to HVIPs is important because many HVIPs lack a sustainable funding source.
“Even if the intervention cost a little more than it saved in dollars and cents to the health care system, there would still be a net benefit in terms of the violence it prevented,” says Purtle.